Pre and Post-operative Care of Intraocular Lens Replacement: An Informative Guide to Cataracts, Lenses, Prevention, and Physics of Refraction
 Anna E. Taiclet
Anna E. Taiclet
As the foremost causative agent to blindness, cataracts of the ocular lens remains a topic of importance within ophthalmologic practices. Although age-related cataracts are the most commonly diagnosed condition within the adult population, visual impairment caused by cataracts can be debilitating to individuals of all ages, including newborns and infants. Performance output may be hindered without an adequate range of vision, concomitant with productivity decline in both the workforce and within a social context1. However, along with rigorous surgical training by medical doctors, technological advancements have aided physicians in reinstating visual capability previously disrupted by cataracts with the procurement of specific instrumentation, and more options for advanced lenses. These factors combined offer patient-specific treatment plans, tailored to each individual’s eye(s), as well as promoting the efficacy of post-operative care.
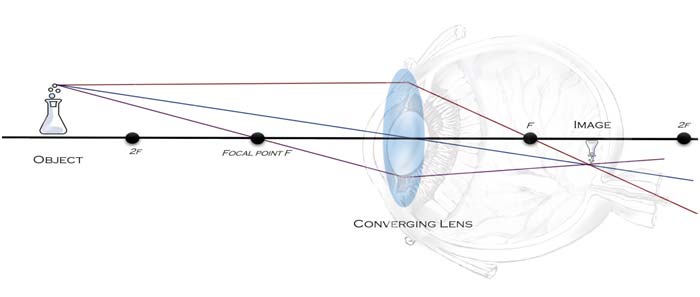
Cataracts occur when the ocular lens loses transparency, impairing light refraction onto the retina of the eye2. Refraction of light occurs when light waves pass through one media to another, for example, the surface of the cornea to the lens of the eye, bending light toward some angle dependent upon the media through which it passes, and the shape of the object refracting it3. The human eye contains a lens that is considered a biconvex structure, which allows the passing of light through the lens, bending or “refracting” the light to a focal point (retina) behind the lights’ point of entry (the lens). When the lens is no longer transparent, light is unable to refract to the retina and yields the typical symptoms described by cataract patients; e.g., blurred vision, a “halo” or “glare” from light sources, or visual impairment in general 1,3.
The onset of age-related cataracts is common in individuals in the mid-forties, early-fifties range. Within the age-related category, three subcategories emerge each possessing a variance in cataract conformation. The first type, nuclear cataracts, is caused directly due to oxidative stress placed upon the epithelial cells of the lens. Not only are these cells the highest in metabolic activity, but the oxidation reactions coupled with crosslinking induces migration of the cells to undergo formation of lens fibers, which constrict the lens (sclerosis) and opacity, or rather a clouded lens. The second form, cortical cataracts, and third, posterior subcapsular cataracts, often occur in conjunction with one another and are observed by direct obscurity of the lens by cell clusters forming a “wedge” (cortical) or an opacity resembling that of plaque (posterior subcapsular) 1,2.
Congenital, or abnormalities formed during gestation prior to birth, cataracts are linked to genetics, X-linked chromosomes, or indeterminable factors. Cataractogenesis is inducible by overuse or long-term use of corticosteroids and other medications (such as phenothiazines), trauma to the eye via physical or chemical accidents, or exposure to radiation such as ultraviolet light. There has been a direct linkage to cataract formation and smoking cigarettes, likely due to the carcinogenic properties associated with cigarette smoking 4.
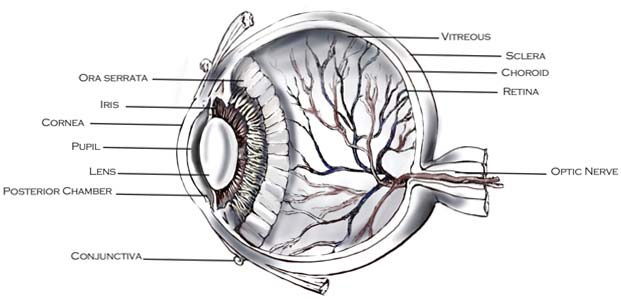
Despite the many factors involved with the onset of cataract formation, the actual percentages of the population who currently have cataracts is decreasing as cataract surgery becomes more cost efficient, and the surgical performance, speed, and postoperative outcomes considerably improve. Surgical techniques to remove cataract lenses have shifted dramatically in replacement methodology; intraocular lenses (IOL) offer a variety of shapes, materials, and visual specificity that was not available during early cataract treatments. A shift from intracapsular and extracapsular extraction towards phacoemulsification techniques, the technique utilized by Tylock Nasser Vision, has not only minimized the invasiveness of removal procedures but limits damage to surrounding tissues as well2. Because the surgical procedure is minimally invasive, it is not necessary, in most situations, to be sedated during lens replacement. Often, the only topical anesthetic is necessary for the procedure, while still maximizing patient comfort.
The phacoemulsification process requires a minimal opening for insertion of an ultrasonic tool, which breaks up the cataract tissue into multiple pieces small enough to be aspirated (suctioned out) from the eye with little damage to surrounding anatomy. Meanwhile, the intraocular space is filled with viscous fluid which maintains the integrity of the eye shape and allows other instrumentation to enter the space without abrasion. The chosen IOL is inserted into space where the cataract had been previously and is able to refract light to the retina without interference by cloudiness. The viscous fluid is then removed, and the new lens is operative immediately. Overnight stay is rarely, if ever, necessary; typically, the procedure only lasts half an hour, perhaps two when considering preoperative evaluations 1,2.
Patients are now given the opportunity to not only choose the lens that best suits their eye physiology (e.g., a lens suitable for fixing astigmatism, or misshapen lens or cornea) but also their visual demands. There are many types of lenses available, and each offers unique results that can be tailored to the patient’s need. Monofocal lenses (such as AcrySof® IQ IOL) possess only one focal point, increasing the ability to see greater distances with more clarity5. Yet, some lenses do not increase visual acuity for closer objects; requiring reading glasses for those activities. Astigmatism-correcting lenses are similar to monofocal lenses, although the physical construction is specific for patients with astigmatism. Multifocal lenses (such as TECNIS® IOL) offer a range of visual acuity at both long and short distances 6.
However, despite increases in performance of physicians and advances in IOL technology, postoperative care is instrumental, and can greatly impact the patient’s adaptation to the new lens. Topical antibiotics (eyedrops) are necessary to reduce the risk of infection following the surgical procedure, and adherence to wearing the protective eye shield is extremely important. Debris and pathogenic species may easily enter the corneal opening without proper postoperative care, despite the minuscule size of the insertion site, and may cause serious issues with visual optimization. Typically, in order to make sure patients are healing correctly, they will be asked to be scheduled for visits one day, one week, and one month following lens replacement. Dependent upon the specificities of the procedure performed, more or fewer appointments may be necessary 1.
Although cataracts still regularly present individuals with visual impairments, surgical procedures, cost, and surgical expertise continue to improve, making the procedure more readily available to the public. As more research and optimization of current protocols continue, cataract replacement surgery will provide bereavement from visual impairments and consequent side-effects.
Reference List
1. Liu Y, Wilkins M, Kim T, Malyugin B, Mehta JS. Cataracts. Lancet, 2017; 390; 600-612.
2. The Eye MD Associates. Lens and cataract: Basic and clinical science course. American Academy of Ophthalmology, 2008; 2008-2009(11); print.
3. Giancoli DC. Physics: Principles with applications. Englewood Cliffs, NJ; Prentice Hall; 2009.
4. Langford-Smith A,Tilakaratna V, Lythgoe PR, Clark SJ, Bishop PN, Day AJ. Age and smoking-related changes in metal ion levels in human lens: Implications for cataract formation. PloS ONE, 2016; 11(1); 1-16.
5. Alcon AcrySof® IR Monofocal IOL: Confidence in the three fundamentals of IOL Performance. Website. https://www.myalcon.com/products/surgical/acrysof-iq-iol/. Updated 2019, accessed March 14th, 2019.
6. Johnson & Johnson Vision Multifocal IOLs: Focus spectacle independence where each patient needs it most. Website. https://www.surgical.jnjvision.com/iols/multifocal. Updated 2019; accessed March 14th, 2019.


